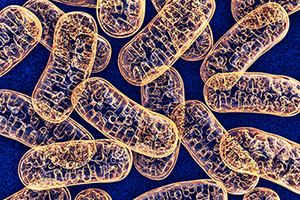
How many of you remember your high school biology?
We all know that our mitochondria are the organelles in our cells that help produce energy for our bodies. Our muscle cells have more mitochondria, which makes sense, but so do our fat cells (as they store the energy).
Once upon a time—around 2 billion years ago—an unprecedented event took place in Earth’s “primordial soup” that teemed with primitive one-celled organisms. An ancient bacterium was engulfed by a larger cell type, perhaps something akin to a forerunner of modern yeast. Instead of being digested, it somehow resisted breakdown and took up residence. In effect, it hitched a ride.
Evolution favored this accident of cooperation because the proto-bacteria had acquired the capacity for cellular respiration (the familiar Krebs cycle that used to bedevil us in organic chemistry class), an advantage over primitive fermentation. More energy could be produced by metabolizing sugar in the presence of oxygen, with a byproduct of CO2.
This enabled future generations of one-celled organisms to become more complex and acquire more specialized functions. Eventually, aggregates of cells like these became the first primitive animals.
This theory is said to explain the origin of mitochondria, the cellular powerhouses in animal cells whose forerunners might originally have been bacteria. They’re so important they have their own DNA, which unlike the rest of our genetic code that partakes equally from our parents, we inherit almost exclusively from our mothers.
Incidentally, this theory about the evolutionary provenance of mitochondria might explain why mitochondria are so vulnerable to the effects of antibiotics.
How your mitochondria are being damaged
What other things can damage mitochondria or impair their function? Free radicals (think smoking!); aging itself (hence the “mitochondrial theory of aging”); chronic inflammation; infections; chemical toxins (e.g. Gulf War Syndrome); nutritional deficiencies; many drugs (e.g. cancer chemotherapy); heavy metals; obesity (Type 2 diabetes is acknowledged to be a form of mitochondrial insufficiency); sedentary lifestyle; high-carb diets; trans fats; and more. In short, many of the features of modern life.
Of course, there are genetic determinants of mitochondrial robustness and resilience. At one extreme are centenarians who retain physical and mental vigor well beyond their peers; at the other are sufferers of a variety of hereditary mitochondrial disorders who must deal with a broad array of brain and body impairments, characterized by extreme weakness, mental retardation, and curtailed longevity.
How much of a leap of imagination is it to posit that most of us ordinary mortals lie on a gradual continuum—without a classic genetic disease, but also not possessors of “super-mitochondria”?
The list of symptoms attributable to impaired mitochondrial function is extensive.
It includes:
- Loss of muscle coordination and weakness
- Problems with vision or hearing
- Learning disabilities
- Heart, liver, or kidney disease
- Gastrointestinal problems
- Neurological problems, including dementia
Other conditions that are thought to involve some degree of mitochondrial dysfunction, include:
- Parkinson’s disease
- Alzheimer’s disease
- Bipolar disorder
- Schizophrenia
- Chronic fatigue syndrome
- Huntington’s disease
- Diabetes
- Autism
- Lyme Disease
And, finally, what you can do about it!
Lifestyle factors that support mitochondria include caloric restriction or intermittent fasting, exercise, exposure to cold, and an anti-inflammatory or Keto diet.
A host of nutritional supplements have been proposed for mitochondrial support: coenzyme Q10 and ubiquinol; L-carnitine and acetyl-l-carnitine; magnesium; B vitamins, selenium, alpha lipoic acid, selenium, zinc, l-taurine, l-arginine, l-citrulline, creatine, melatonin, vitamin C, vitamin K3, vitamin E, caffeine, pyrroloquinoline quinone (PQQ), D-ribose, and alpha keto glutarate to name some of the most plausible.
But here I’d like to concentrate on just two of special interest, one old, one new.
NT Factor came onto my radar screen in the 90s when it was proposed as a treatment for debilitation. I tried it out on one of my most bedraggled patients—a long-term cancer sufferer who was reeling from the aftereffects of chemo. To my surprise, he rallied, and went on to experience many months of good quality-of-life. Subsequent positive experiences with fatigued patients turned me into a believer.
The principle behind NT Factor is “lipid replacement therapy” (LRT) as described by Garth Nicholson Ph.D. It’s a glycophospholipid that is said to repair and fortify cell membranes.
In addition to the lipid bilayer that encapsulates cells, specialized membranes surround mitochondria, and also serve as “assembly lines” within them for electron transport reactions linked to energy production. “Ragged” membranes are thought to be a hallmark of damaged or senescent mitochondria, hence NT Factor’s role in restoring efficient energy metabolism.
Clinical trials have supported the efficacy of NT Factor for post-chemo fatigue, general debilitation, Chronic Fatigue Syndrome, fibromyalgia and chronic Lyme Disease, and Gulf War Syndrome.
Two capsules daily of Healthy Aging—the dose I take—delivers 1300 mg of pure NT Factor along with a “mitochondrial fuel blend”. Individuals suffering challenging fatigue issues might do well to take 4 or even 6 capsules per day to attain dosages used in clinical trials with sick patients.
The other supplement I recommend to support healthy mitochondria is new: nicotinamide riboside. It’s long been recognized that vitamin B3–in its niacin and niacinamide forms—is an essential precursor to NAD+. Nicotinamide adenine dinucleotide (NAD+) acts an electron transport molecule, shuttling electrons within the mitochondria the way copper wires deliver electricity to your appliances.
In addition to providing energy, NAD promotes the sirtuin pathway, associated with the beneficial effects of calorie restriction. By consuming NAD, sirtuins can regulate a whole range of cellular processes, including those associated with mitochondrial biogenesis.
A decline in NAD+ has been associated with aging and a variety of health conditions. We lose up to 50% of our NAD+ levels between the ages of 40 and 60. While supplementing with vitamin B3 has been proposed as a strategy for addressing age-related decline, newer research suggests it is not the best approach for boosting NAD+.
NAD cannot be given as a supplement, so efforts have focused on developing precursor compounds that boost NAD+ in the cells. In 2004, a landmark study by Dr. Charles Brenner uncovered a unique form of vitamin B3 that can raise NAD levels in human cells. Since then, clinical trials have demonstrated that nicotinamide riboside, in doses easily attainable via oral administration, boosts cellular NAD+ in human subjects.
Interest in nicotinamide riboside has skyrocketed since its introduction, with over 100 research studies exploring its potential, and many more underway. Possible efficacy has been seen in a wide range of tissues and conditions, though most of these trials have been performed in test tube or animal models with further testing in humans still needed. Several human trials have been completed and more are in process.
TruNiagen®️ is the brand of nicotinamide riboside I recommend to patients because it’s the original product developed by Dr. Brenner, who currently serves as Chief Scientific Advisor to Chromadex. For maintenance, it’s recommended that you take 2 capsules of TruNiagen 150 mg daily. For those who want the highest dose available per capsule, I recommend TruNiagen Pro 300 mg (the highest potency available on the marketplace) 2 capsules daily.